A multitude of just-in-time home and community-based services at your fingertips.
We are a network of mission-driven organizations that operate a complex service delivery system providing statewide access to community-based, in-home services to more than 300,000 older Ohioans and people with disabilities. Simply put, we’ve helped countless people return to the comforts of home and stay there. We’ve achieved those results through a range of services that address needs from all angles. We can achieve these results for you and your members.

Assessments
Upfront and follow-up sessions to understand a participant’s risk level, social determinants of health, and program eligibility.

Person Centered Planning
Determination of the recommended benefits based on the clinical need and/or social determinants impacting clinical outcomes and connecting members and caregivers to services.

Hospital to Home Care
Patient-focused interventions that assist in the shift between care settings to ensure a seamless system of support for participants and caregivers.

Care Coordination
Coordination of support services that prevent or postpone institutionalization and avoid unnecessary hospitalizations. Create plans that enable your members to exit nursing home care, even after prolonged institutionalization.

Caregiver Supports
Tools and education that maintain the stability of the member’s support system including caregiver support and respite care service.

Home Delivered Meals and Nutritional Supports
Targeted in-person home-delivered meals in order to address the risk of food insecurity and reducing the risk of readmissions related to reduced nutritional intake.

Transportation
Coordinate non-emergency medical transportation to health appointments and non-medical transportation to combat social isolation.

Homemaker and Personal Care
Maintaining a clean, safe and healthy living environment with assistance for general household activities and personal care services in the home.
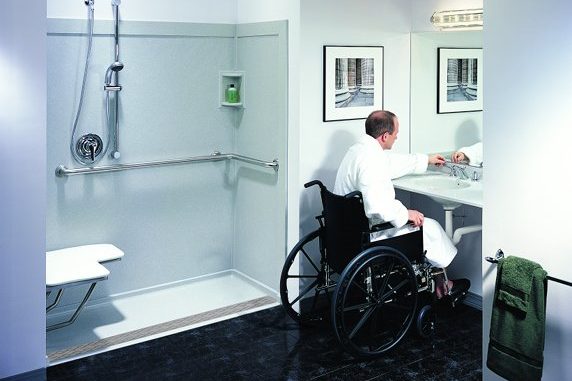
Home Modifications
Home and bathroom safety device and accessibility improvements installation.

Health and Wellness Programs
Education and outreach to promote healthy living practices for better aging outcomes and the management of chronic illness such as diabetes.

Provider Network Management
Centralized IT system and billing, and contract management and payment that ensures quality and streamlines efficiency.
STAY AT HOME
Members can remain at home longer and delay or avoid expensive nursing home stays.
AVOIDING READMISSIONS
Avoid unnecessary and hospital admission and readmission and emergency room visits.
MEMBER SATISFACTION
Provides ability to target benefits to meet members’ needs.
Latest News
Addressing Social Determinants: Scaling Up Partnerships With Community-Based Organization Networks
A new Health Affairs blog post highlights the growing capacity of aging and disability community-based organizations to address the social determinants of health (SDOH). Ohio’s Area Agency on Aging network[…]
Read moreArea agencies on aging address elders’ health needs where they live
“There is often a disconnect between the worlds of health care and social services, with each sometimes having different goals, different terminology and different ways of being paid. But individuals[…]
Read moreMedicare spends more on socially isolated older adults
A study conducted by Stanford University and AARP Public Policy Institute found that a lack of social contacts among older adults is associated with an estimated $6.7 billion in Medicare[…]
Read more